UC Davis professor involved in research team conducting largest study of U.S. access to 3D mammography
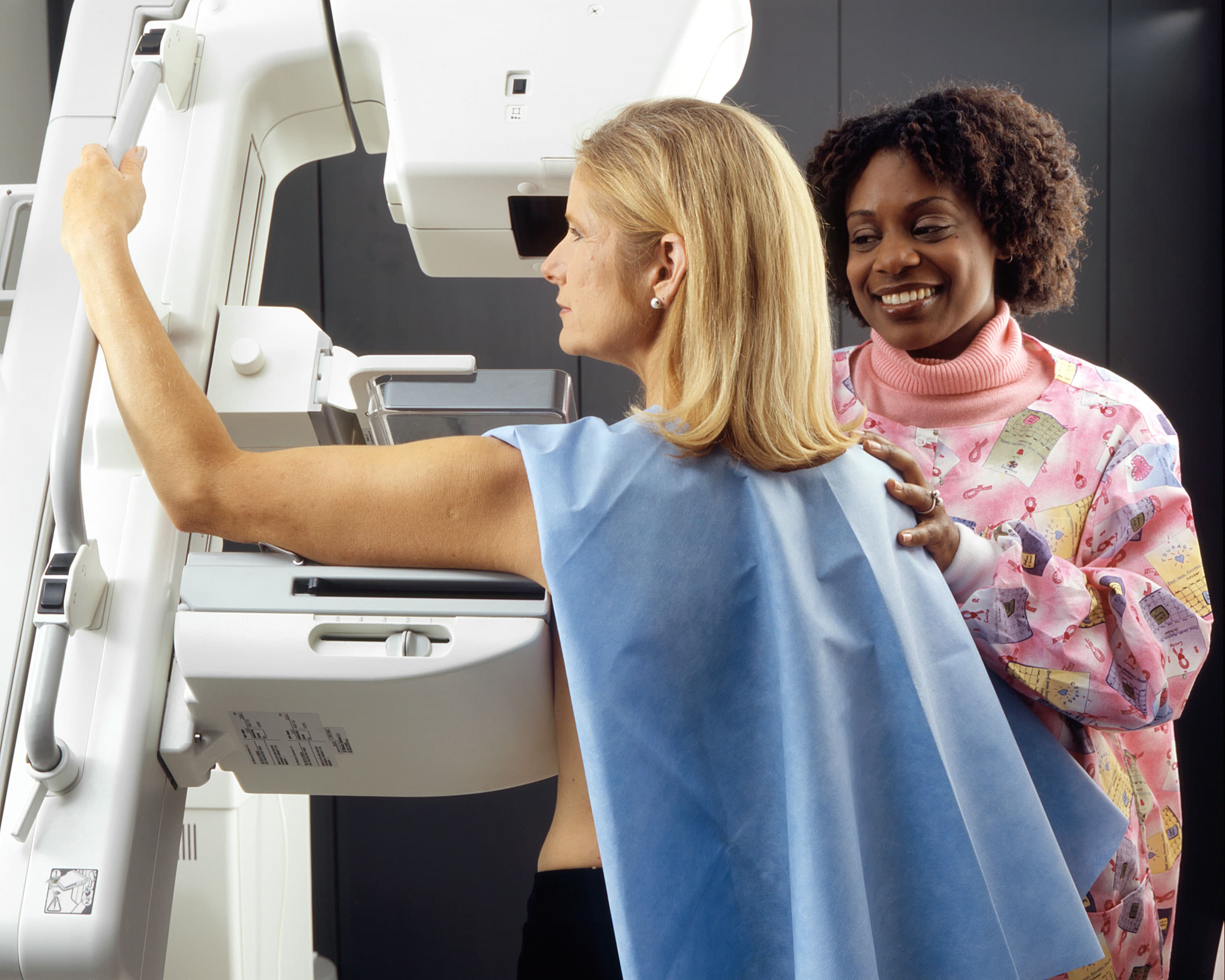

Breast screening exams from the Breast Cancer Surveillance Consortium reveal disparities in access to improved detection technologies
UC Davis School of Medicine Professor and Division Chief of Biostatistics Diana Miglioretti was among a team of researchers that conducted a cross-sectional study recently published in JAMA Network Open. Researchers evaluated accessibility to, and usage of, digital breast tomosynthesis (DBT) based on a variety of factors including race, ethnicity, education and income.
“We were concerned that new technologies could widen persistent disparities in breast cancer mortality if there isn’t equitable uptake by facilities accessed by underserved communities,” Miglioretti said via email.
According to the author contributions of the study, Miglioretti was involved in developing the concept and design of the study, acquiring data, conducting statistical analysis, interpreting the results, obtaining funding and supervising.
Miglioretti has a personal connection to her research that makes early detection of cancer especially important to her.
“My great-grandmother died of breast cancer in her early 30s and my grandmother and aunt were both diagnosed with breast cancer in their 40s,” Miglioretti said. “All eligible individuals in the US should have access to high-quality screening and follow-up care.”
According to the study, prospective trials and observational studies reveal that DBT, also known as 3-dimensional mammography, can be used to improve breast cancer screening outcomes when compared to digital mammography, more commonly known as DM, or 2-dimensional mammography.
DBT is a “relatively new technology,” according to a FAQ published by the FDA.
“3D mammography improves screening performance through lower false positive rates and small increases in cancer detection for some subgroups of individuals,” Miglioretti said. “If underserved communities do not have access to this new technology, they do not get to benefit from these improvements.”
Professor of Radiology at the University of Washington School of Medicine Christoph Lee said that underserved populations are usually the last to have access to new medical technologies.
“If 3D mammography does not diffuse into clinical settings in an equitable fashion, then differential technology adoption could exacerbate existing screening outcome disparities,” Lee said via email.
The results of the study lead to the general conclusion that women of minority races and ethnicities along with those of lower socioeconomic statuses have less access to DBT screening.
“Access to the best diagnostic tools for detecting breast cancer shouldn’t depend on your zip code or your income level,” said Associate Professor of Radiology at the UC Davis School of Medicine and Chief of the Breast Imaging Section Shadi Aminololama-Shakeri, via email. “That’s why this type of research is critical to enveil existing healthcare disparities. Only then can we start to address these inequalities and help patients access the latest lifesaving screening technology that gives us the best chance at detecting cancer.”
In particular, only 37.7% of Black women, 44% of Hispanic women, and 42.8% of Asian Americans were able to acquire DBT when both screening technologies were available.
Additionally, while 50.6% of women with a college degree obtained DBT, only 40.8% of women with less than a highschool diploma were able to access this technology.
“It is important to identify inequalities in the diffusion of new technologies so that healthcare providers, policy makers and advocacy groups can focus on ways to ensure more equitable access to these technologies,” Miglioretti said.
Similarly, only 43.9% of women living in zip codes associated with the lowest income quartiles obtained DBT in comparison to the 51.4% of women in the highest income quartile.
“We need more clear guidance on what subpopulations of women are most likely to benefit from 3D mammography, and to lower barriers to access for these women,” Lee said. “These include providing evidence to third-party payers for clinical effectiveness of 3D mammography in specific populations.”
These results were determined from approximately 2.3 million “routine screening mammography examinations among women aged 40 to 89 years,” collected from 92 imaging facilities in five different states between Jan. 1, 2011 and Dec. 31, 2017, according to the study. This data was provided by the Breast Cancer Surveillance Consortium.
“The Breast Cancer Surveillance Consortium is unique in that all of their facilities prospectively collect very detailed woman-level information at each imaging exam,” Lee said. “This allowed us to associate individual social determinants of health with their exam-level outcomes.”
Miglioretti said classifying individuals as coming from an underserved community proved to be a challenging task.
“We used crude measures based on self-reported race/ethnicity and education and geocoded measures of income and rural/urban residence,” Miglioretti said. “In future research, we would like to evaluate other measures of social determinants of health including measures of structural racism.”
Miglioretti said that one of her top priorities is providing high-quality health care for all by ensuring each individual has access to high-quality screening, follow-up and treatment.
“At UC Davis, 3D mammography is available to every woman who walks through our doors,” Shakeri said.
Written by: Aarya Gupta — science@theaggie.org
