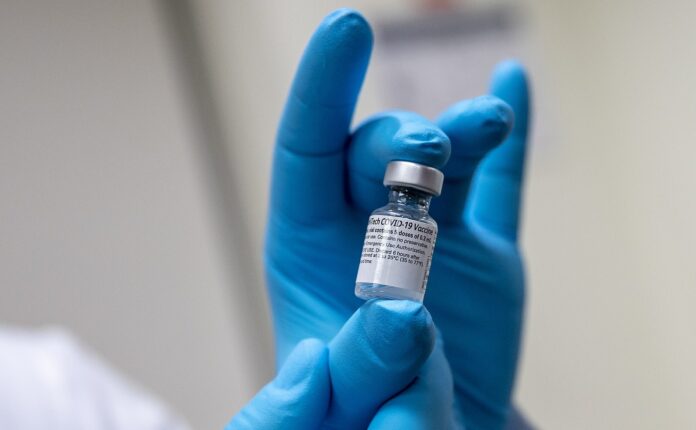
60 of 225 participants from original COVID-19 vaccine trial return to UC Davis Medical Center
As of Aug. 20, the Centers for Disease Control and Prevention (CDC) recommends that “people who are moderately to severely immunocompromised should receive an additional dose of mRNA COVID-19 vaccine after the initial 2 doses,” according to their website.
Professor and Chair of Internal Medicine at UC Davis Health Dr. Timothy Albertson explains that the vaccines developed by Pfizer Inc. and Moderna Inc. are examples of messenger RNA (mRNA) vaccines.
According to the CDC’s website, COVID-19 mRNA vaccines provide instructions to cells to make “harmless […] spike proteins.”
“MRNA is put in lipid spherules, injected and entered into the cell, which makes the spike protein,” Albertson said. “That spike protein is pushed out of human cells, and then antibodies are formed to that spike protein.”
The immune system recognizes the spike proteins on the surface of cells and begins building a response by producing antibodies, according to the CDC.
“In vaccination, you are harnessing the immune system of the body to generate a response against a pathogen,” said Dr. Angela Haczku, the associate dean for translational Research at UC Davis Health. “In this case, [the pathogen] is the SARS-CoV-2 virus. The way the vaccine accomplishes [this] is through activating immune cells and getting them to produce immunoglobulins against the virus.”
While this process occurs through natural COVID-19 infection, the CDC said that those who are vaccinated “gain this protection without ever having to risk the serious consequences of getting sick with COVID-19.”
“The immune activation, if it is repeated, generates a much greater response than a single or dual activation step, which is provided by the first [or second] doses,” Haczku said. “A third, or booster, shot would boost your immune system to produce even more protection against the virus.”
Haczku said that unlike certain childhood vaccinations, where one shot is enough to induce lifetime immunity, current COVID-19 vaccinations only accomplish shorter protections.
“We don’t know exactly how long this protection is at the moment, because there have never been any studies for that,” Haczku said. “One of the main purposes of this third shot trial is to gain information on the effectiveness of such a booster shot.”
Starting from July 2020, UC Davis Medical Center became one of 150 sites participating in a global clinical trial that investigated the efficacy and side effects of the COVID-19 mRNA vaccine manufactured by Pfizer Inc. and BioNTech SE, according to an article published by UC Davis Health.
The data collected at this time resulted in the Food and Drug Administration issuing an Emergency Use Authorization (EUA) in December 2020 for this vaccine, Albertson said.
“[We were selected to participate] because of our reputation for clinical trials and the excellence of the investigators and clinical trial coordinators,” Haczku said.
Haczku said that at any time UC Davis can juggle about 500 active clinical trials at once.
Clinical Research Coordinator at UC Davis Medical Center Gabby Echt adds that UC Davis’ Medical Center’s success with this original trial can also largely be attributed to the high volume of enrollment and the rich diversity within the population it serves.
“The Sacramento area is very diverse in terms of ethnicity and socioeconomics,” Echt said. “As a researcher, I value the importance of promoting diversity in clinical trials so that people of many backgrounds are represented in research, especially during a time like this—where everything is a bit scary, and people might be hesitant to trust the healthcare system when they need it the most.”
Now, 60 of the 225 volunteers that participated in this original clinical have returned for this booster trial. Echt describes this trial to be a “one-year, double-blind, placebo-controlled study.” This means that half of the participants received a placebo, or a saline or salt-water solution, while the other half received BNT162b2, which is the Pfizer vaccine.
“The booster is made up of the exact same components and dosage of the original Pfizer vaccine,” Echt said. “It is just a third injection of the vaccine.”
Assignment was random, and both participants and the research staff were unaware of which treatment each participant received.
“This is necessary so that we would be able to assess the effects of the actual vaccines,” Haczku said. “If this booster shot is effective, those volunteers that received the placebo, instead of the third injection, will also have the opportunity to get vaccinated a third time.”
Albertson said that the process of collecting multifactorial data—including antibody levels, infection levels and reactivity to the third dose—has been “remarkably straightforward.”
“We’re following their antibody levels,” Albertson said. “We’re following whether they get COVID-19 or not with self-swabbing and a daily diary. It is hugely important to determine whether or not a third vaccine is needed. We have some indirect evidence out there that it is. Our patients are relatively healthy. We’re looking to see if the general public needs that. We think that might be the case.”
Echt said that researchers are still waiting for the interim analysis for the booster trial to be released by Pfizer Inc.
“This is a trial that will take a couple of months,” Haczku said. “The investigators and the volunteers are blinded. So, until the results are revealed, we won’t be able to tell if this third shot works.”
Regardless, researchers remain hopeful.
“People have been incredibly brave and dedicated,” Albertson said. “Recognize that people participating in clinical trials are heros. They made a commitment way before anybody had a clue as to how safe these drugs were. Understand that this particular Pfizer drug has been given to probably a billion people worldwide […] which is an incredible number for a pharmaceutical drug. The risks are incredibly small and the benefits are incredibly large to be vaccinated.”
Written by: Aarya Gupta — science@theaggie.org